The deadlift is a popular strength training exercise that involves lifting a weighted barbell off the floor to a standing hip position. However, it is also one of the most debated exercises due to concerns about risk of injury, with plenty of misinformation across the internet. Does the evidence support deadlifting for low back pain patients under a professional’s guidance? Is it an all-or-nothing exercise where the risks outweigh the benefits? Let’s unpack these questions and more!
Deadlifts ≠ automatic injury
First, examining injury rates will provide us some insight. Weightlifters do show a higher incidence of back injuries compared to other athletes, with deadlifting as a common precipitating factor(1). Not surprising that the people doing it the most are more likely to face injuries. However, a 2020 systematic review found that in trained lifters, deadlift injury rates are low at just 0-5.9%(2). Aside from good recovery practices that emphasize sleep and nutrition, proper progressive loading and technique can help to minimize injury risk(3).
What about for people with back pain?
Individuals with low back pain often experience limitations in their ability to perform daily activities or participate in recreational or sports-related endeavors. For these folks, research increasingly supports deadlift retraining under supervision. Several studies demonstrate the deadlift can reduce pain and disability when added to physical therapy programs. A 2015 study had patients follow a 16-week rehab protocol of mobility exercises plus hip hinge movements progressing to deadlifts. 83% saw clinically meaningful improvements in pain and function(4). A 2018 randomized controlled trial added deadlifts to standard PT care for 3 months. The deadlift group improved significantly more than controls on pain and disability scores(5).
These benefits are thought to occur because deadlifts dynamically load and strengthen the spine’s supporting musculature in a safe, controlled manner(6). Proper form also trains coordinated hinging movement patterns useful for everyday activities. Simply put, the deadlift is a functional exercise for all!
Ideal strategies to consider when utilizing the deadlift in a rehab program

- It may be helpful to supplement a client’s program with graded loading and baseline mobility, stability, and movement pattern training (7)
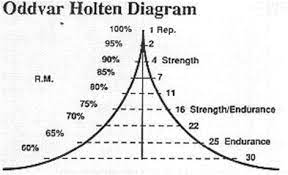
- Use low loads and high repetitions if needed initially – no maximal lifts early on, especially to clients new to this lift (8)
- Closely monitor form, provide cues, and avoid overloading (9)
- Equally as important to the above, allow the client to safely explore nuances in technique and positioning. This will build confidence and adaptation to the exercise while building injury resilience.
- Progress slowly over 8+ weeks up to heavier loads based on response (10)
While more research is still needed, evidence indicates deadlifts can play a helpful role in rehab for low back pain under proper PT guidance and load management. No exercise is ever risk-free, but deadlifts performed correctly offer unique benefits that may outweigh their potential risks for select clients.
If you have a new or nagging injury or are not sure where to start, book a FREE discovery session (in person or virtual) with one of our Doctors of Physical Therapy!
Please note: The content in this blog is intended for educational purposes only and is not medical advice. See a healthcare professional if you have any questions about your individual needs.
References:
1. Raske A, Norlin R. Injury incidence and prevalence among elite weight and power lifters. Am J Sports Med. 2002;30(2):248-256. doi:10.1177/03635465020300020601
2. Calhoon G, Fry AC. Injury rates and profiles of elite competitive weightlifters. J Athl Train. 1999;34(3):232-238.
3. Siewe J, Rudat J, Röllinghoff M, et al. Injuries and overuse syndromes in powerlifting. Int J Sports Med. 2011;32(9):703-711. doi:10.1055/s-0031-1277207
4. Kim D, Cho M, Park Y, Yang Y. Effect of lumbar stabilization and dynamic lumbar strengthening exercises in patients with chronic low back pain. Ann Rehabil Med. 2015;39(1):110-117. doi:10.5535/arm.2015.39.1.110
5. Steele J, Bruce-Low S, Smith D. A Rehabilitation Program That Integrates Modified Resistance Training and Motor Control Retraining in Chronic Low Back Pain Patients Improves Muscular Endurance, Strength, and Pain: A Randomized Controlled Trial. BioMed Research International. 2015;2015:1-8. doi:10.1155/2015/30764
6. McGill S. Low back stability: from formal description to issues for performance and rehabilitation. Exerc Sport Sci Rev. 2001;29(1):26-31. doi:10.1097/00003677-200101000-00006
7. Hales M, Johnson BF, Johnson JT. Kinematic analysis of the powerlifting style squat and the conventional deadlift during competition: is there a cross-over effect between lifts?. J Strength Cond Res. 2009;23(9):2574-2580. doi:10.1519/JSC.0b013e3181bc191a
8. Schoenfeld BJ, Grgic J, Ogborn D, Krieger JW. Strength and Hypertrophy Adaptations Between Low- vs. High-Load Resistance Training: A Systematic Review and Meta-analysis. J Strength Cond Res. 2017;31(12):3508-3523. doi:10.1519/JSC.0000000000002200
9. Swinton PA, Stewart A, Agouris I, Keogh JW, Lloyd R. A biomechanical analysis of straight and hexagonal barbell deadlifts using submaximal loads. J Strength Cond Res. 2011;25(7):2000-2009. doi:10.1519/JSC.0b013e3181e73f87
10. Contreras B, Vigotsky AD, Schoenfeld BJ, Beardsley C, Cronin J. A comparison of gluteus maximus, biceps femoris, and vastus lateralis electromyography amplitude in the parallel, full, and front squat variations in resistance-trained females. J Appl Biomech. 2016;32(1):16-22. doi:10.1123/jab.2015-0194